Discover the featured content in this month’s The Annals of Thoracic Surgery issue, personally selected by Editor-in-Chief Dr. Joanna Chikwe & Senior Editor Dr. Robbin Cohen, who highlight the authors' important findings, with select illustrations from Dr. Sarah Chen, Associate Editor/CMI. As an additional benefit to your STS Membership and Annals subscription, this monthly newsletter aims to bring expert perspectives on recently published research, straight to your digital doorstep.
Featured in the June 2026 issue...
STS Document | The Society of Thoracic Surgeons (2025) Expert Consensus Document on Interventions for Screen-Detected Lung Nodules
Servais, Shrager, and coauthors
The STS Task Force on Lung Cancer Screening and the Workforce on Evidence-Based Surgery convened a multidisciplinary panel to create 23 consensus statements describing quality standards for CT lung cancer screening programs. Key points of the consensus statements include the following:
- Surgery without tissue diagnosis is acceptable for selected patients, favoring minimally invasive, parenchymal-sparing techniques.
- Programs should track benign resection rates.
- Definitive resection should occur within 12 weeks of the inciting imaging study.
- Complication benchmarks for bronchoscopic biopsy included pneumothorax <5%, hemoptysis <2%, and mortality <1%.
- Surgical morbidity should be <10% and mortality <1%.
- Multidisciplinary teams should include thoracic surgery, oncology, pulmonology, and radiology.
-Robbin Cohen, MD, MMM
Senior Editor
Lung | Wedge Resection for Early-Stage Non-Small Cell Lung Cancer: Are We There Yet?
Baiu, Kneuertz, and coauthors
This review synthesizes the available evidence comparing wedge resection with segmentectomy for the surgical treatment of early-stage non-small cell lung cancer, referencing lobectomy as the historical benchmark. The authors provide a detailed discussion regarding the evidence for sub-lobar resection, a comparison of wedge resection vs. segmentectomy using established trials, and a summary of ongoing trials. The technical and biologic considerations that must be considered when performing wedge resection are discussed to ensure that clinical results are comparable to anatomic resections. These include functional status of the patient, impact of margin distance, quality of lymph node dissection, tumor biology, and the presence of additional lung nodules.
-Robbin Cohen, MD, MMM
Senior Editor
Lung | Comparing Nodal Upstaging Rates and Morbidity and Mortality of Common Nodal Sampling Guidelines in the STS General Thoracic Surgery Database
Potter, Yang, and coauthors
The 2026 Richard E. Clark Memorial Paper for General Thoracic Surgery queried the STS General Thoracic Surgery Database to compare lymph node sampling strategies regarding nodal upstaging and M&M in patients undergoing surgical resection for clinical stage I-IIIA non-small cell lung cancer between 2021 and 2024. Of 46,954 patients, 68.7% met the American College of Surgeons Commission on Cancer Operative Standard 5.8 (sampling of >3 mediastinal and >1 hilar), 32.4% met a modified European Society for Thoracic Surgery lobe specific guideline, 25.9% met a modified Japanese lobe specific guideline, 83.9% met a “2+1” guideline (>2 mediastinal and >1 lobar), and 16.1% met no guideline. Whereas nodal upstaging rates were similar for all staging strategies (11.5%-11.7%), patients who met no guidelines had a significantly smaller chance of nodal upstaging. M&M rates were nearly identical across the four guidelines, and similar to those among patients who met no guidelines.
-Robbin Cohen, MD, MMM
Senior Editor
Aorta | Outcomes of Staged Completion Extent II Thoracoabdominal Aortic Aneurysm Repair
Ikeno, Estrera, and coauthors
This retrospective study compared primary (181 pts, 62.4%) vs. staged (109 pts, 37.6%) extent II TAAA repairs at a high-volume aortic center between 1999 and 2024. Operative mortality, respiratory failure, dialysis requirement, early SCI and stroke rates were comparable between the two procedures, though delayed SCI was twice as high with primary repair. A summary of initial procedures and the extent of repairs contributing to staged operations is seen in this figure from the article:
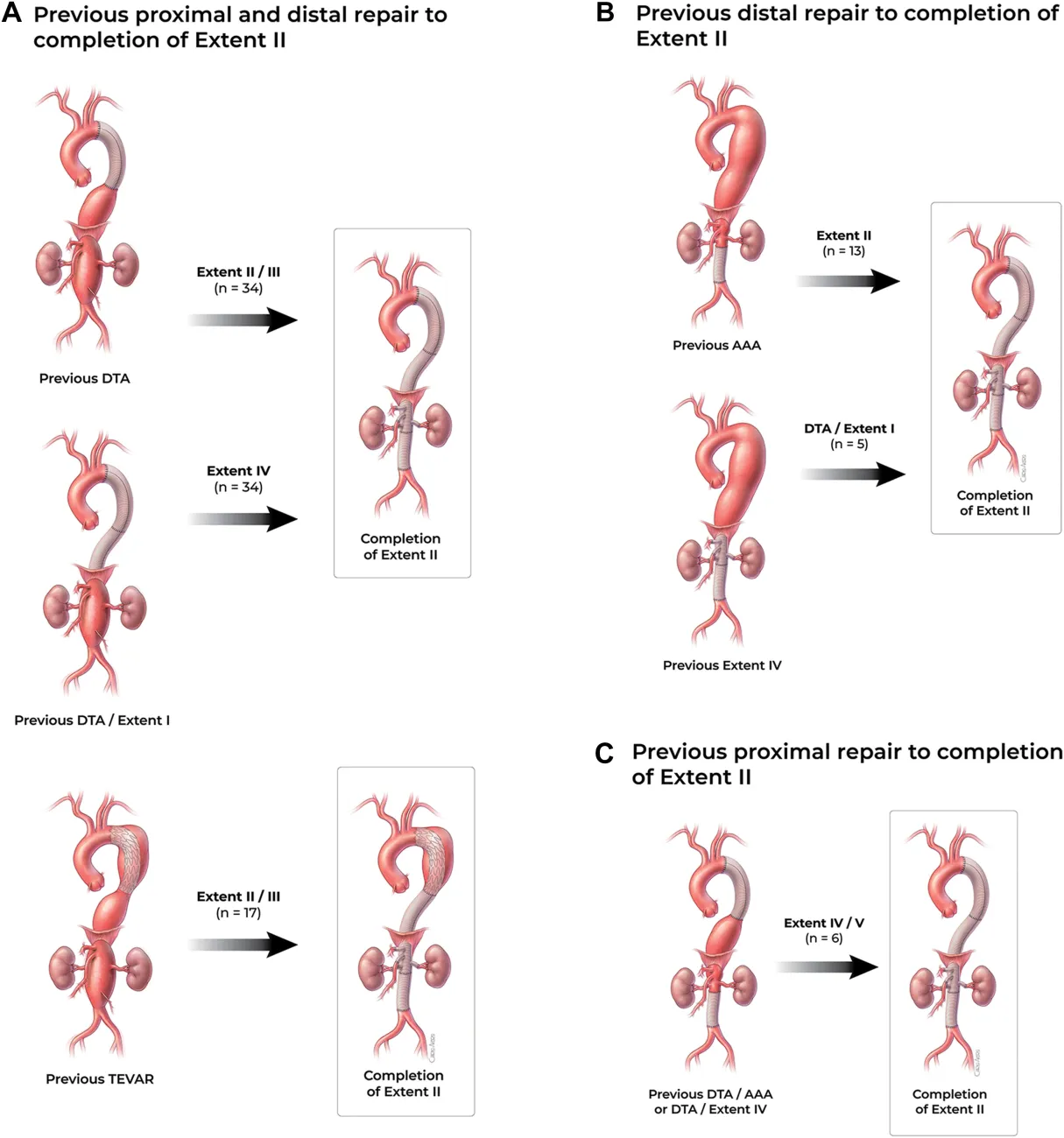
-Robbin Cohen, MD, MMM
Senior Editor
Coronary | Risk-Adjusted Outcomes of Reoperative vs Primary Coronary Artery Bypass Grafting
Radakovic, Deutsch, and coauthors
This single center retrospective review of isolated CABG procedures compared 12,120 first time CABGs with 341 redo-CABG procedures between 2009 and 2023. Crude in-hospital mortality was 1% in primary CABG vs. 1.8% in redo CABG. After risk-score matching (258 pairs); in hospital mortality, stroke, myocardial infarction, hemofiltration, and ECMO rates were similar between the two groups. Though survival at up to 10 years was also comparable, there was a higher need for repeat revascularization in the redo CABG group. The authors attribute their excellent results with redo CABG to high volume experience, detailed preoperative evaluation and imaging, thorough assessment of available conduits, and strategic operative planning.
-Robbin Cohen, MD, MMM
Senior Editor
Valve | Long-Term Outcomes of Repeated Transcatheter Aortic Valve Replacement vs Transcatheter Aortic Valve Replacement Explantation: A Nationwide Analysis
Faggion Vinholo, Sabe, and coauthors
Using national administrative claims data from the Centers for Medicare & Medicaid Services (CMS), the authors evaluated long-term outcomes of repeated TAVR versus TAVR explantation in Medicare patients with bioprosthetic valve dysfunction following an initial TAVR procedure. Among 1172 patients, repeated TAVR was more common (70.6%) and associated with lower short-term mortality, while TAVR explantation (29.4%) provided better survival at 3 and 5 years. Survival curves crossed at about 9 months, after which explantation showed sustained benefit, even across varying comorbidity levels. The findings highlight that, although repeated TAVR is less risky in the short term, TAVR explantation may offer superior long-term outcomes for certain patients.
-Joanna Chikwe, MD
Editor-in-Chief
Valve | Increasing but Variable Use of Surgical Treatment of Atrial Fibrillation: An Update from The STS Adult Cardiac Surgery Database
Hodges, Cox, and coauthors
Following The Society of Thoracic Surgeons 2023 Clinical Practice Guidelines for the Surgical Treatment of Atrial Fibrillation (AF), which recommends concomitant surgical ablation and left atrial appendage occlusion (LAAO) for patients with AF undergoing cardiac surgery, this study uses recent data from the STS Adult Cardiac Surgery Database on over 1.2 million patients. The authors found that while the rate of untreated AF declined (42.4% to 24.8%) and isolated LAAO increased (14.7% to 30.1%), surgical ablation rates remained stagnant. Variability in AF treatment was observed based on patient characteristics, surgery type, region, surgeon, and program volume. Despite progress, significant variability and undertreatment persist, highlighting the need for targeted education, monitoring, and quality metrics.
-Joanna Chikwe, MD
Editor-in-Chief
Congenital & Pediatric | Risk Factors and Outcomes for Infants Requiring Unplanned Reintervention after Stage 2 Palliation for Single-Ventricle Heart Disease
Krishnan, Chan, and coauthors
This retrospective analysis of the National Pediatric Cardiology Quality Improvement Collaborative database looked at 2095 patients who underwent stage 2 palliation for single-ventricle heart disease, of which 401 patients (19.1%) had unplanned reintervention. Reinterventions included interventional catheterization only (247 pts), surgery only (78 pts), and both catheterization and surgical intervention (76 pts). Risk factors for unplanned reintervention included hybrid as stage 1, reintervention after stage 1, tube feedings at stage 2, and additional cardiac procedures during stage 2 surgery. Patients who underwent both surgical and catheterization reinterventions had a median 21-day longer stay and underwent additional reinterventions between stage 2 discharge and first birthday. Any reintervention was associated with decreased transplant free survival (hazard ratio, 2.2; 95% CI, 1.4-3.5).
-Robbin Cohen, MD, MMM
Senior Editor
Transplant & Mechanical Support | Survival After Left Ventricular Assist Device: A Society of Thoracic Surgeons National Intermacs Database Risk Model Assessment
Mehaffey, Kirklin, and coauthors
This retrospective study utilized the STS National Intermacs Database and machine learning multivariable oblique random survival forests to compare 3 models predicting 3-year survival after LVAD implantation. Three cohorts of patients who received LVADs from 2013-2023 were defined. Cohort 1 included fully magnetic devices only (12,449 pts, 2018-2023). Cohort 2 included hydrodynamic and magnetically levitated and axial flow devices (CF/AF) from 2018-2023 (3235 pts), and cohort 3 CF/AF from 2013-2017 (14,019 pts). For analysis, Model 1 included only cohort 1; Model 2 included cohorts 1 and 2; and model 3 combined all three cohorts. Three-year survival after LVAD implantation was 71.5% for patients with fully magnetic devices (cohort 1) and 58% for cohort 2 (p<.0001). Model discrimination was similar across all 3 models, whereas model calibration was superior in model 1.
-Robbin Cohen, MD, MMM
Senior Editor
