STS News, Winter 2019 -- Four new e-learning modules are available as part of the Society’s effort to create relevant online continuing education materials for cardiothoracic surgeons and their teams.
The topics were chosen after a careful review of continuing medical education (CME) requirements from each state medical board in the United States. Certain states mandate that physicians complete CME in specific topic areas, so STS leaders took those mandates into account and also considered which subjects would most directly impact cardiothoracic surgeons and their patients—now and in the future.
These modules, on surgical ethics, shared decision-making, breaking bad news, and cultural competencies, can be accessed via the STS Learning Center (sts.org/learningcenter). Each will take approximately 30 minutes to complete, and users will be eligible for either CME credit or a certificate of participation.

The surgical ethics module presents several scenarios that may not have straightforward answers.
Surgical Ethics
A wide variety of clinical situations present ethical difficulties in surgery. The surgical ethics module addresses four questions related to uses and abuses of technology:
- Should a patient be given an unindicated transcatheter aortic valve replacement before an impending loss of insurance?
- Does an iatrogenic injury require that an otherwise futile procedure be done?
- Can a surgeon refuse to operate on an intravenous drug-abusing patient with recurrent aortic prosthesis infection?
- Is an experienced surgeon performing a robotic lobectomy for the first time ethically obligated to include his/her limited experience in the informed consent discussion?
“The e-learning module on surgical ethics helps surgeons analyze a variety of difficult situations in which more than one option may seem reasonable, or in which there is disagreement between the surgeon and patient or family on how to proceed,” said one of the module developers, Robert M. Sade, MD, former Chair of the STS Committee on Standards and Ethics and the 2012 recipient of the Society’s Distinguished Service Award.
“The e-learning module on surgical ethics helps surgeons analyze a variety of difficult situations in which more than one option may seem reasonable.”
Shared Decision-Making
The shared decision-making module helps cardiothoracic surgeons understand the importance of involving patients when making decisions about treatment options.
“Surgeons need education to overcome misconceptions about shared decision-making; there are several inhibitors to its adoption,” said James R. Edgerton, MD, a member of the Society’s Clinical Practice and Member Engagement Council Operating Board who helped create the module. “Surgeons may believe that the practice will lead to incorrect decisions or that they don’t have the time for it. Further, they simply may not be familiar with the process. But a patient’s active participation is a key factor in establishing a strong physician-patient relationship and may improve outcomes.”
The module looks at three scenarios that may be challenging, especially for a surgeon who is new at shared decision-making:
- A 45-year-old diabetic woman with complex coronary disease is afraid of pain from a sternotomy and wants a minimally invasive procedure combined with medical therapy, which the surgeon feels is a poor decision.
- A 50-year-old man diagnosed with a stage I non–small-cell carcinoma in his lung chooses to forgo the surgeon’s recommended treatment because he’s worried about losing his job if he takes too much time off from work.
- An 87-year-old man who experienced a postoperative stroke has become ventilator- and dialysis-dependent; the surgeon recommends that his wife withdraw aggressive care, but she is unable to make the decision.
The module also explores factors that impact a patient’s ability to participate in shared decision-making, including age, socioeconomic status, and disease status. Surgeons will be given tools and techniques to aid patients in the process.
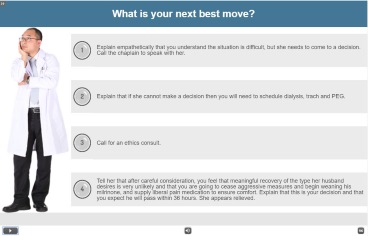
The e-learning modules challenge users to apply the information they’ve learned.
Breaking Bad News
The breaking bad news module provides guidance on discussing end-of-life care with patients and their families. It outlines a complicated situation in which a patient’s advanced directive gave medical power of attorney to his wife, who had been institutionalized for several years with dementia.
Surgeons will be provided with specific steps to take and language to use when they encounter similarly challenging situations in the future.
Cultural Competencies
The cultural competencies module examines how surgeons can deliver care that addresses not only patients’ medical needs, but also their social and cultural needs. It addresses topics such as sensitivity to religion, gender differences, distrust of the health system, and language barriers.
“As cardiothoracic surgeons, we need to have a better understanding of our patients’ expectations based on their beliefs so that optimal care is delivered,” said Subroto Paul, MD, MPH, one of the module developers.
To purchase the modules, visit sts.org/learningcenter. If you have questions, contact the STS Education Department.