STS News, Winter 2022 — Projects funded through the Society’s charitable arm, The Thoracic Surgery Foundation (TSF), are igniting discoveries that improve the lives of patients and keep cardiothoracic surgeons at the helm of research.
TSF research grant recipient Paul Chun Yung Tang, MD, PhD, is utilizing the lab at the University of Michigan Frankel Cardiovascular Center in Ann Arbor, to explore a better way to ensure that donor hearts serve their recipients well after transplant.

“Currently—and this has been the case for decades—when you want to preserve hearts, you use a specific formulation of electrolytes and buffers to keep them cold and stop it from beating,” Dr. Tang said. “We stop the heart from beating so it’s using less energy, and we hope that we’ve achieved a state of cryostasis. Our research has shown that’s probably not entirely the case. There are a lot of molecular events slowly happening while in ice and the heart may be programmed to misbehave even before you put it in.”
During transport and cold storage, donor hearts may suffer from the stress of lost blood flow, and consequentially from deprivation of oxygen and nutrients. This stress can result in oxidative stress and the release of inflammatory molecules that may inhibit the heart’s function once blood flow is restored.
Dr. Tang’s team proposed that infusing valproic acid (VPA), a histone deacetylase inhibitor, into donor hearts during the harvesting process could reduce oxidative stress and inhibit the release of inflammatory molecules during storage, resulting in improved function when the heart resumes beating.
To explore this proposition, Dr. Tang needed a laboratory, he needed hearts, and he needed funding. The Frankel Cardiovascular Center has an excellent environment for the development of clinical and translational science programs, Dr. Tang explained in his TSF grant proposal.
He identified The Gift of Life Michigan organ procurement facility in Ann Arbor, a 15-minute drive from the lab, as a resource that could provide approximately 50 human donor hearts per year for research purposes. And in 2018, Dr. Tang was awarded a TSF Southern Thoracic Surgical Association Resident Research Award, which supplied $25,000 toward the project.
Dr. Tang’s team worked on pig hearts and also collected human donor hearts with a left ventricular ejection fraction between 50% and 65%, but not suitable for clinical transplantation due to issues such as advanced donor age or cardiac hypertrophy. They then preserved the hearts with either traditional histidine-tryptophan-ketoglutarate (HTK) solution alone or with HTK plus VPA.
At various points during cold preservation and mechanical arrest, the investigators collected left ventricular (LV) and right ventricular (RV) tissue samples, and they performed RNA sequencing and differential gene analysis to characterize gene expression and regulation in the two groups. They examined responses related to muscle contraction, cardiac conduction, and gluconeogenesis, as well as cellular apoptosis, innate immune responses, and metabolomic processes.
“We discovered that VPA was able to intervene in some of the metabolic processes and selectively harness the protective metabolites that make the heart more resilient to ischemic injury,” Dr. Tang said. “VPA treatment downregulated the expression of apoptosis-related genes and the expression transcripts related to immune activation during the hypothermic preservation. And it was able to upregulate antioxidant proteins, which would predict improved cardiac function,” continued Dr. Tang. “So VPA appears to have highly beneficial effects in terms of gene expression.”
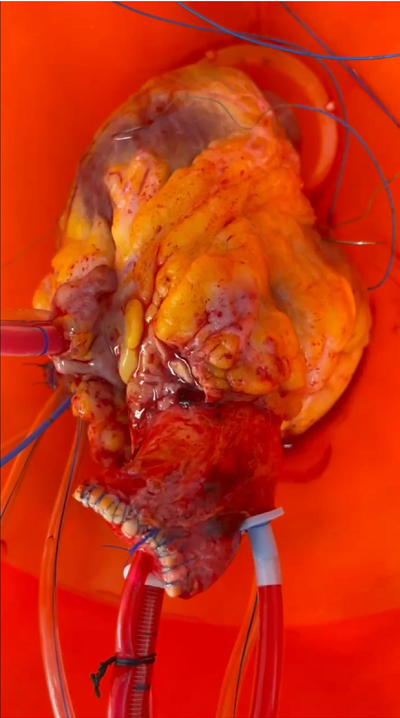
For measuring cardiac performance after revival, the team used human and pig hearts, perfused with HTK solution with or without VPA. “Our experiments showed that, in the heart that was only cold preserved with HTK solution for a prolonged period, there was poor contractility and frequent arrhythmias,” Dr. Tang noted. “It required multiple shocks throughout the ex-vivo perfusion run because we had repeated episodes of ventricular fibrillation and tachycardia. After 2 to 3 hours, this heart was unable to maintain a sinus rhythm and continually fibrillated.”
The pig heart treated with both HTK and VPA, on the other hand, stayed strong after revival, maintaining a sinus rhythm. “It was shocked once at the very beginning of ex-vivo perfusion and reanimation, and it maintained a good rhythm and contractility for the perfusion period,” said Dr. Tang.
These promising initial results have spurred additional experiments. Also, Dr. Tang is assembling a proposal for further funding from the National Institutes of Health, and he emphasizes that receiving initial seed funding from programs like TSF—and having intriguing preliminary research funded through this pathway—make him a more attractive candidate for larger-scale grants.
“It’s critical to seek out a program that’s supportive of translational research, and that’s willing to provide the initial funds to at least get your lab started,” Dr. Tang added. “If research is a worthwhile avenue for you, any dedicated research time you can get will help you advance your goals.”
Scan the QR code to watch the researchers' videos of reanimated hearts with and without molecular modulation.


Virtual Fun Run Merges Charity with Camaraderie
The TSF Virtual Fun Run & Walk, held in conjunction with STS 2022 in Miami Beach, Florida, gives attendees and supporters an exciting way to support the Foundation and compete with colleagues. This virtual race allows participants to join the fun from anywhere in the world, anytime from January 21–February 1.
Runners and walkers can complete the challenge solo or as part of a team—and teams can be groups of patients, hospital employees, friends, family, exhibitors, or corporate staff. All are welcome.
Individuals can register for $50 USD, and a Team Captain Sponsorship of $500 USD may include up to 11 registrations. All proceeds will benefit TSF cardiothoracic research programs. Participants can track their time and compete with other individuals and teams, or complete the course at their own pace.
Race results will be displayed on the STS leaderboard and shared on social media with the #STS2022 and #TSF5K hashtags.